Ketamine Clinics
Anesthesiologists and pain physicians operate most of the Ketamine clinic.
Both of these groups possess experience with this medication and make natural low-dose Ketamine treatment clinicians.
Despite this, anyone with a license to prescribe can write for intravenous or intranasal Ketamine. For instance, many psychiatrists are now entering the industry.
Ketamine clinical treatment centers focusing on mental health can offer a collection of modalities such as transcranial magnetic stimulation (TMS), pharmacotherapy (psychiatric medication), and Ketamine Assistive Therapy (KAT).
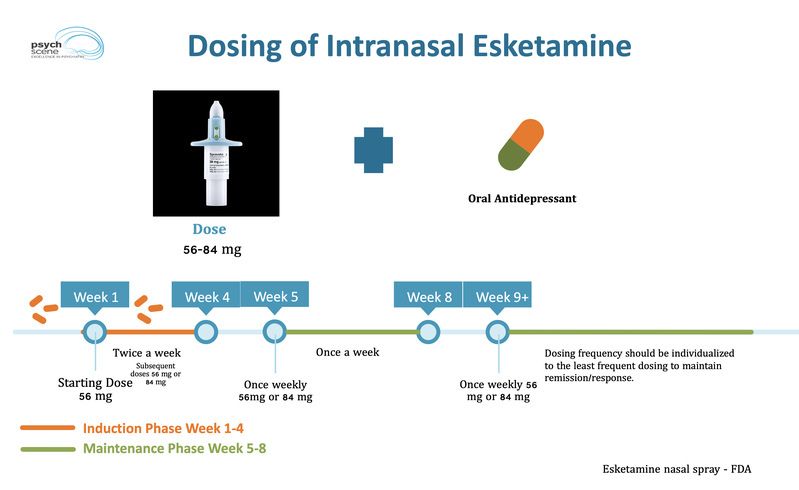
Now that esketamine, the nasal spray brand-named Spravato is FDA approved and covered by insurance for depression, it too is joining the clinical offerings.
Where to get Ketamine?
The number of Ketamine clinics in the United States is mushrooming – estimated at more than 400. Explosive growth necessitates regulation and standard operating procedures.
Procedures include steps for screening patients for contraindicated conditions and substance abuse history, assessing candidacy per diagnosis, coordination with the patient’s external medical team, informed consent, dosage calculation, safety monitoring, and protocols for minimizing adverse effects.
Deploying a Ketamine registry could provide a larger swath of data to inform these efforts. A comprehensive data gathering effort with ketamine clinics is difficult to coordinate.
Is Ketamine legal?
Due to its classification as “experimental,” infusions of Ketamine are rarely covered by insurance.
It is still legally prescribed, but applying it outside of anesthesia and pain, is considered “off label.” Off-label use simply means that a drug may help with conditions not officially indicated by the FDA.
Treating physicians supply off-label prescriptions at their discretion. Further, referrals to receive Ketamine treatment are not necessary in most cases, reducing the friction for care.
Esketamine
The “mirror molecule” of Ketamine, esketamine (brand name Spravato), was approved in 2019.
IV infusions require significant infrastructure to administer. It’s believed that a nasal spray can make treatments more convenient and accessible in a wider variety of settings.
While ketamine has a long track record as an anesthetic and pain reliever, esketamine lacks that history.
Whether Ketamine is superior to esketamine therapeutically or safety-wise will unfold over time.
For now, it presents an affordable treatment option for a desperate patient population.
What is Esketamine nasal spray?
The high cost of ketamine is a barrier to many patients, who are already financially disadvantaged due to their health problems. This situation may perpetuate health disparities.
However, once the FDA approved Spravato intranasal spray for cases of major depression not responding to standard treatment, hope emerged.
FDA approval kicked off the march to insurance covering esketamine prescriptions. Copays remain but are dramatically less than the several hundred dollars attached to low dose IV Ketamine infusion therapy.
Esketamine vs Ketamine
IV Ketamine infusions trace back to the 1960s. Much is known about their effects, mechanisms of action, and side effects. Esketamine does not have this history to draw from.
Esketamine nasal spray is not the same as racemic Ketamine as that used in infusions and surgery.
Racemic Ketamine infusions combine both sides of the mirror molecule, both “R” and “S.”
Esketamine is only the “S” isomer. These molecules are frequently discussed interchangeably – this is incorrect and problematic.
Why are the differences important?
The isomers exhibit different properties; meaning the S and K, whether used together in a particular ratio or separately, behave differently.
While there are overlapping properties, each has its idiosyncratic particulars of symptoms relieved and associated side effects.